
Your primary physician has determined that colonoscopy is necessary for further evaluation or treatment of your condition. This brochure has been prepared to help you understand the procedure. It includes answers to questions patients most frequently ask. Please read it carefully. If you have additional questions, please feel free to call our Center. To paraphrase a New York retailer, a well-informed patient is our best customer. We strive to provide individual care in a non-rushed, but efficient manner. We have great respect for our patients and make colonoscopy a “non-event.” There is nothing embarrassing about colonoscopy and its proper performance can have a dramatic effect on your life.
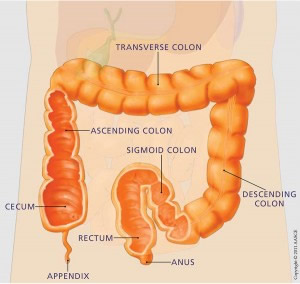 The colon, also called the large intestine, is a six-foot long organ that works to absorb water from the intestinal tract and help store and then deliver bowel movements. Ingested food first traverses the stomach where it is solubilized. Liquefied food then moves to the small intestine and this portion of the intestinal tract acts to absorb nutrients. Fluids then proceed to the colon where stool is solidified as water is absorbed. The beginning of the colon is located in the right lower portion of the abdomen. It comes up the right side and crosses the abdomen under the diaphragm and then drops down the left side of the abdomen into the pelvis and the rectum.
The colon, also called the large intestine, is a six-foot long organ that works to absorb water from the intestinal tract and help store and then deliver bowel movements. Ingested food first traverses the stomach where it is solubilized. Liquefied food then moves to the small intestine and this portion of the intestinal tract acts to absorb nutrients. Fluids then proceed to the colon where stool is solidified as water is absorbed. The beginning of the colon is located in the right lower portion of the abdomen. It comes up the right side and crosses the abdomen under the diaphragm and then drops down the left side of the abdomen into the pelvis and the rectum.
During colonoscopy, a flexible instrument is inserted into the rectum and is advanced throughout the colon. The patient is lying on their left side during the exam. The instrument has a video camera built into its tip and the image of the lining of the colon is projected to a television screen. The instrument is the diameter of an index finger. The Center uses state-of-the-art equipment and presently uses high definition endoscopes. The procedure generally takes 20-30 minutes to perform. Occasionally procedures take longer especially if polyps are encountered. During colonoscopy, biopsies can be obtained from anything abnormal and polyps can be removed. This is all done during the same exam.
The colon is the site of the second most common cancer killer in America. The small intestine is an unusual site for cancer. Most colon cancer begins in benign growths called polyps. These bits of tissue can grow over years and then degenerate into cancer. Most polyps are easily removed during colonoscopy, thus reducing the future risk of cancer.
Other diseases that effect the colon include infections or chronic inflammatory illnesses that produce diarrhea, broken blood vessels that can cause bleeding and diverticular disease that in a minority of patients can lead to pain, infection or bleeding. Hemorrhoids can also be seen and assessed during colonoscopy, though surgical treatment requires the intervention of a proctologist and thus is not performed during colonoscopy.
Another way to examine part of the colon is sigmoidoscopy. In this exam, a shorter instrument examines the bottom most portion of the colon called the sigmoid and that is how the exam got its name. This exam requires a less extensive preparation and patients are not usually sedated for the exam.
A newer exam is virtual colonoscopy. In this exam, the same preparation for standard colonoscopy is required. A patient has a small tube inserted in the rectum and air is instilled. A CAT scan is then performed. The pictures obtained can be similar to pictures at colonoscopy. This exam does not allow biopsing of tissue. Polyps cannot be removed and if they are found, standard colonoscopy is required.
Colonoscopy is usually well tolerated and rarely causes pain. The lining of the colon can only sense distention. Unlike the nerves in your hand, there are no nerve endings in the colon that can sense temperature, touch, or pain. Air is instilled during colonoscopy to distend the bowel and allow adequate examination. This can produce the sensation of abdominal pressure. The air is removed prior to the completion of the exam. Patients are sedated prior to starting the exam. There is no standard dose of sedation and the amounts given are individualized. More medication can always be given during the exam.
The colon must be completely clean for the procedure to be accurate and complete. A liquid diet a day prior to the exam is required followed by an oral purgative that cleanses the colon. Enemas are not necessary. Your physician will provide you with detailed instructions for the preparation in separate literature. The preparation will vary according to your medical history and the timing of your exam.
Most medications may be continued, but some medications can interfere with the preparation or the examination. Blood thinners, insulin and iron products are examples of such medications. You should notify the Center of all medications that you take as well as any medication allergies you have. Do not stop aspirin or Plavix prior to colonoscopy. You should alert the Center if you require antibiotics prior to undergoing dental procedures, since you may need antibiotics prior to colonoscopy as well.
You will rest following the completion of the exam. Generally, patients are able to leave the Center 20 to 30 minutes after the exam. You will be able to leave under your own power. You will be able to eat immediately after the exam and food will help you eliminate any remaining effects of the sedation medications. There will not be any dietary restrictions. You cannot drive a car for 8 hours or drink alcohol for 8 hours after the examination.
Your physician will meet with you after the exam and results will be provided immediately. Results of any tissue sent for pathologic evaluation are usually available after 3 business days. Our Center will call you in several days to make sure you are well and provide the opportunity to ask any remaining questions. A full written report will be sent to your primary physician.
Colonoscopy and polypectomy are extremely safe. Possible complications include bleeding from a polypectomy site and perforation of the colon wall. Bleeding is usually minor and stops on its’ own or can be controlled through the colonoscope. Only rarely are blood transfusions or surgery required. Perforation is extremely uncommon during a normal exam and when it does rarely happen, it is usually associated with attempts to remove large polyps or tumors. Perforation requires immediate surgery.
Although complications after colonoscopy are uncommon, it is important that you recognize early signs of any possible complication. Notify the Center if you have severe abdominal pain, fever and chills, or rectal bleeding of more than one-half cup. Bleeding can occur several days after polypectomy.
There are specific federal guidelines for cleaning endoscopic equipment. The Center closely adheres to all of these guidelines. All equipment is manually scrubbed and then placed in an automatic disinfection unit.